Electronic Fetal Monitoring | Vibepedia
Electronic fetal monitoring (EFM) is a medical technology used to track the heart rate of a fetus and the mother's uterine contractions during pregnancy and…
Contents
Overview
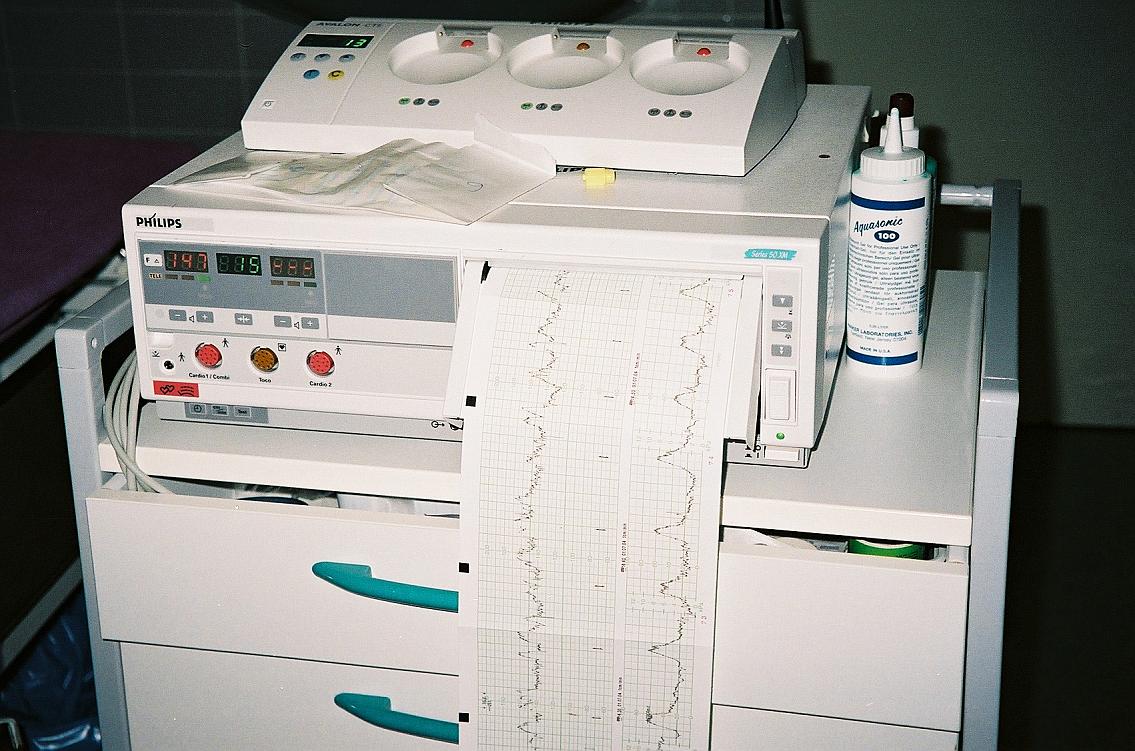
Electronic fetal monitoring (EFM) is a medical technology used to track the heart rate of a fetus and the mother's uterine contractions during pregnancy and labor. Employing external transducers placed on the abdomen or internal electrodes attached to the fetus, EFM provides a continuous visual record, typically displayed as a graph on a screen or printed strip. Developed in the mid-20th century, its primary aim is to detect fetal distress, particularly hypoxia, and guide clinical interventions to improve birth outcomes. Despite its widespread adoption, EFM remains a subject of significant debate regarding its efficacy in preventing stillbirths and neurological injury, with ongoing discussions about optimal interpretation and application, particularly in low-risk pregnancies.
🎵 Origins & History
The roots of electronic fetal monitoring (EFM) stretch back centuries, with early attempts to discern fetal heart sounds using rudimentary devices. By the mid-19th century, the Pinard horn, a type of acoustic stethoscope, allowed for intermittent auscultation of the fetal heartbeat. The development of continuous electronic monitoring began in the 1950s and 1960s, laying the groundwork for its clinical application. This shift was fueled by a growing desire to proactively identify and manage fetal distress during labor, a critical concern in obstetrics.
⚙️ How It Works
Electronic fetal monitoring typically involves two primary methods: external and internal. External monitoring uses tocodynamometer belts placed on the mother's abdomen to detect uterine contractions and Doppler ultrasound transducers to capture the fetal heart rate. These signals are transmitted to a cardiotocograph machine, which displays the data as two superimposed tracing lines on a screen or paper. Internal monitoring, employed when a clearer signal is needed or external methods are insufficient, involves a sterile spiral electrode attached to the fetal scalp and an intrauterine pressure catheter inserted into the uterus. These invasive methods provide more precise data on fetal heart rate and contraction intensity, though they carry a small risk of infection or injury to the fetus. The interpretation of these tracings, often categorized by baseline rate, variability, accelerations, and decelerations, is crucial for assessing fetal well-being.
📊 Key Facts & Numbers
The use of EFM varies globally. Studies have shown that while EFM use has increased, its impact on reducing perinatal mortality rates has been debated. The cost of EFM equipment and associated training for healthcare professionals represents a substantial investment for healthcare systems. Despite its prevalence, the rate of cesarean sections has continued to rise in many countries, prompting questions about the role EFM plays in these surgical interventions.
👥 Key People & Organizations
The development of EFM is linked to several key figures and institutions. Early pioneers laid the groundwork for continuous electronic monitoring. Major medical device manufacturers like Hewlett-Packard (now Philips Healthcare) and GE Healthcare have been instrumental in commercializing and refining EFM technology, making it accessible to hospitals worldwide. Professional organizations such as the American College of Obstetricians and Gynecologists (ACOG) and the Society for Maternal-Fetal Medicine (SMFM) play a crucial role in establishing guidelines for its use and interpretation.
🌍 Cultural Impact & Influence
Electronic fetal monitoring has profoundly reshaped the cultural perception of childbirth, transforming it from a purely natural event into a medically managed process. The visual representation of the fetal heartbeat on a screen has become an iconic image of modern obstetrics, symbolizing vigilance and technological intervention. This constant surveillance has, for some, increased anxiety during labor, while for others, it provides reassurance. EFM has also influenced legal landscapes, with EFM tracings frequently becoming central evidence in malpractice lawsuits concerning birth injuries. Furthermore, the widespread adoption of EFM has contributed to a broader trend of medicalization in childbirth, influencing patient expectations and the roles of midwives and obstetricians in the delivery room. The very definition of a 'safe' birth has, in many societies, become intertwined with the use of such monitoring technologies.
⚡ Current State & Latest Developments
The current landscape of EFM is characterized by incremental technological advancements and ongoing efforts to refine interpretation protocols. Newer systems offer wireless monitoring, allowing greater maternal mobility during labor, a significant departure from the tethered machines of the past. Artificial intelligence (AI) is increasingly being explored to assist in the real-time analysis of fetal heart rate tracings, aiming to improve accuracy and reduce inter-observer variability. Despite these innovations, the core principles of monitoring and the debates surrounding its efficacy persist. The focus remains on optimizing its use, particularly in identifying true fetal distress while minimizing unnecessary interventions like cesarean sections and operative vaginal deliveries.
🤔 Controversies & Debates
The most persistent controversy surrounding EFM revolves around its effectiveness in preventing adverse outcomes, particularly cerebral palsy and stillbirth. While critics argue that EFM detection does not consistently translate into improved neurological outcomes and may lead to a higher rate of interventions without clear benefit. The National Institute for Health and Care Excellence (NICE) in the UK, for example, has issued guidelines that recommend intermittent auscultation for low-risk labors, reserving continuous EFM for higher-risk situations, a stance that contrasts with the more routine use in some other countries. The interpretation of EFM tracings themselves is also a point of contention, with significant variability among clinicians, leading to potential misinterpretations and differing clinical decisions. The financial implications of widespread EFM use, including equipment costs and potential litigation, also fuel debate.
🔮 Future Outlook & Predictions
The future of EFM is likely to be shaped by advancements in wearable technology and artificial intelligence. We can anticipate more sophisticated, non-invasive sensors that offer greater maternal freedom of movement and potentially integrate other physiological data. AI algorithms will likely become more sophisticated, moving beyond simple pattern recognition to predictive analytics, identifying fetuses at risk of distress hours or even days in advance. This could lead to more personalized and proactive obstetric care. However, the fundamental question of whether continuous electronic monitoring is the optimal strategy for all pregnancies, or if it should be reserved for specific indications, will continue to be a subject of research and clinical debate. The push for evidence-based practice may lead to more nuanced guidelines, potentially reducing routine EFM in low-risk populations globally.
💡 Practical Applications
Electronic fetal monitoring finds its primary application in antepartum and intrapartum care. Antepartum monitoring, conducted before labor, is typically used for high-risk pregnancies, such as those with gestational diabetes, preeclampsia, or [[intrauterine-growth-re
Key Facts
- Category
- technology
- Type
- topic