Finger Prick Glucose Meters | Vibepedia
Finger prick glucose meters, also known as blood glucose meters (BGMs), are portable electronic devices used to measure the concentration of glucose in the…
Contents
Overview
The genesis of the finger prick glucose meter can be traced back to the mid-20th century, a period when blood glucose measurement was largely confined to clinical laboratories. Early attempts involved cumbersome chemical tests that were impractical for home use. The breakthrough came with the development of electrochemical biosensors. The Ames Company, a division of Miles Laboratories, introduced the first portable, self-monitoring blood glucose meter. This device required a larger blood sample and was still relatively complex. However, it paved the way for miniaturization and improved accuracy. By the 1980s, meters like the Accu-Chek from Roche Diagnostics and the One Touch from LifeScan (then part of Johnson & Johnson) began to emerge, utilizing smaller blood samples and simpler test strips, making home monitoring a viable reality for many people with diabetes. The development of enzyme-based test strips, particularly those using glucose oxidase, was a pivotal moment, enabling more precise readings.
⚙️ How It Works
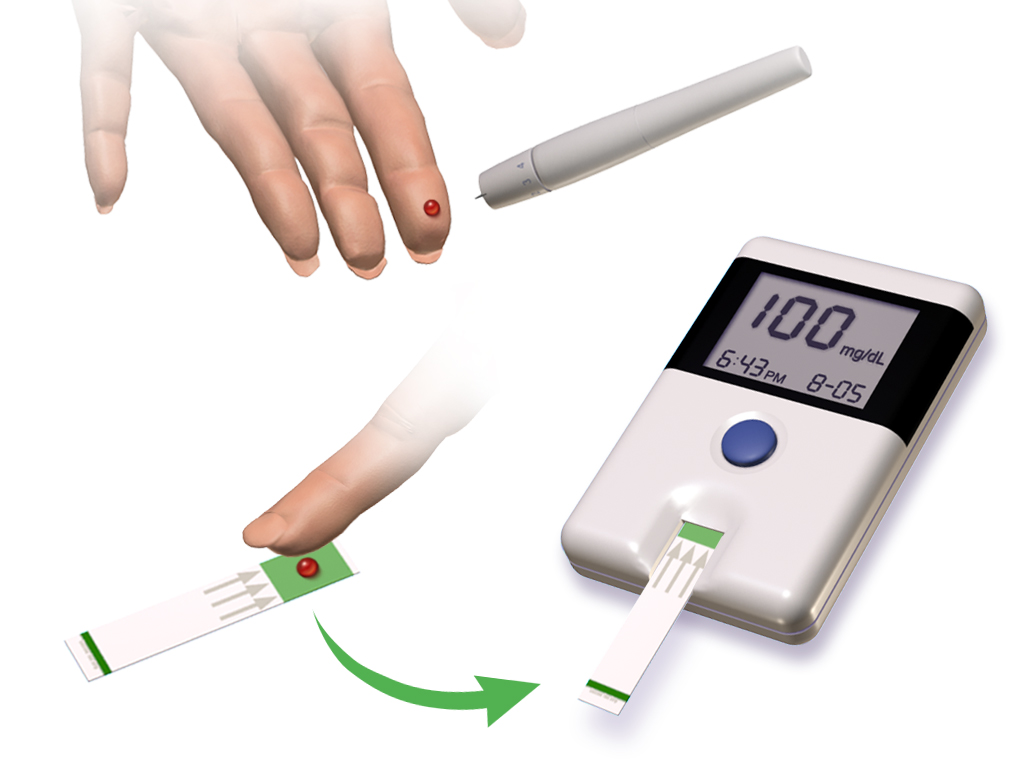
At its core, a finger prick glucose meter operates on electrochemical principles. The process begins with a lancet, a small needle, piercing the skin, typically on a fingertip, to obtain a tiny droplet of capillary blood. This blood sample is then applied to a disposable test strip, which contains enzymes (commonly glucose oxidase or glucose dehydrogenase) and other chemicals. When glucose in the blood interacts with the enzyme, a chemical reaction occurs, producing an electrical current or a color change. The meter then measures this electrical signal or analyzes the color intensity using optical sensors. This measurement is translated into a blood glucose reading. The accuracy of the meter depends on the quality of the test strip, the calibration of the meter, and the user's technique, as highlighted by organizations like the American Diabetes Association.
📊 Key Facts & Numbers
The scale of finger prick glucose meter usage is staggering. The cost of these meters can range widely, but the ongoing expense of test strips represents a substantial financial burden for many users. In the United States, Medicare alone covers millions of glucose meters and billions of test strips each year, illustrating the significant healthcare expenditure associated with this technology.
👥 Key People & Organizations
Several key individuals and organizations have shaped the landscape of finger prick glucose meters. Dr. Arnold Kadish is credited with inventing the first portable blood glucose meter. Roche Diagnostics has been a consistent innovator, launching its Accu-Chek line of meters early on. LifeScan, a former Johnson & Johnson subsidiary, became a dominant player with its One Touch meters. Abbott Diagnostics is another major manufacturer, known for its FreeStyle line. The American Diabetes Association and the International Diabetes Federation play crucial roles in setting guidelines for diabetes management, including recommendations for blood glucose monitoring, and advocating for patient access to these essential devices. Regulatory bodies like the U.S. Food and Drug Administration (FDA) also play a critical role in ensuring the safety and efficacy of these devices.
🌍 Cultural Impact & Influence
Finger prick glucose meters have profoundly democratized diabetes care, transforming it from a clinical-only concern to a daily, personal responsibility. The ability to test blood glucose at home, in real-time, has empowered individuals to make immediate dietary, exercise, or medication adjustments, leading to better glycemic control and a reduction in severe hypoglycemic and hyperglycemic events. This technology has also fueled a vast ecosystem of diabetes education, support groups, and online communities where individuals share experiences and tips related to meter usage and data interpretation. The visual representation of blood glucose numbers on a meter screen has become a tangible, often anxiety-inducing, but ultimately vital, metric for millions, influencing lifestyle choices and fostering a deeper understanding of their bodies' responses. The widespread adoption of these meters has also influenced public health campaigns and awareness initiatives surrounding diabetes.
⚡ Current State & Latest Developments
The market for finger prick glucose meters remains robust, though it faces increasing competition from continuous glucose monitoring (CGM) systems like those from Dexcom and Abbott Diagnostics's FreeStyle Libre. Manufacturers continue to refine their BGM offerings, focusing on smaller blood sample sizes, faster test times (some now under 5 seconds), improved accuracy, and enhanced connectivity features. For instance, newer meters often offer Bluetooth capabilities to sync data with smartphone apps, facilitating easier tracking and sharing with healthcare providers. The development of integrated lancet devices and strips that require minimal handling has also improved user convenience. Despite the technological advancements in CGM, the lower cost of BGMs and test strips ensures their continued relevance, particularly in low- and middle-income countries and for individuals who find CGM technology inaccessible or overly complex.
🤔 Controversies & Debates
The primary controversy surrounding finger prick glucose meters centers on accuracy and accessibility. While modern meters are generally accurate, discrepancies can arise due to factors like user error, strip degradation, environmental conditions, or inherent limitations of the technology (e.g., interference from certain medications or substances). Some studies have questioned the accuracy of certain meters, particularly in specific patient populations or under challenging conditions, leading to debates about regulatory standards and manufacturer claims. Another significant debate revolves around the cost of test strips. For many individuals, especially those without adequate insurance coverage, the ongoing expense of test strips can be prohibitive, leading to dangerous practices like rationing strips or skipping tests altogether. This has fueled calls for greater price transparency and affordability initiatives from manufacturers and policymakers. The transition to CGM also raises questions about equitable access to newer, more expensive technologies.
🔮 Future Outlook & Predictions
The future of finger prick glucose meters is likely one of co-existence and integration rather than outright replacement by CGMs. Manufacturers will continue to push the boundaries of accuracy, speed, and user-friendliness. We can expect to see more meters with advanced connectivity, allowing seamless data transfer to electronic health records and sophisticated diabetes management platforms. Integration with artificial intelligence (AI) for predictive analytics and personalized feedback is also on the horizon, potentially offering users insights beyond simple glucose readings. Furthermore, efforts to reduce the cost of test strips and meters will be crucial to maintain their accessibility, especially in global markets. It's also plausible that some meters will incorporate additional biomarker testing capabilities, moving beyond just glucose to offer a more comprehensive health snapshot from a single drop of blood, potentially competing with other diagnostic point-of-care devices.
💡 Practical Applications
Finger prick glucose meters have a wide array of practical applications, primarily centered around diabe
Key Facts
- Category
- technology
- Type
- topic